General Cardiology Research
Using Qualitative Research in Applied Clinical Research

Qualitative research methodologies enable researchers to explore a diverse range of topics that provide valuable insights into various healthcare and caregiving contexts where quantitative data is unavailable. Researchers can uncover nuanced perspectives, experiences, and meanings that contribute to a deeper understanding of complex issues in healthcare. Qualitative findings can complement quantitative work, inform development of hypotheses, and be part of development or evaluation of clinical interventions. These publications showcase Dr. Harrison’s application of qualitative methods in understanding dementia/caregiver experiences, healthcare resource allocation, palliative care needs, and more.
First Author
- Harrison KL, Garrett SB, et al. "I Didn't Sign Up for This": Perspectives from Persons Living with Dementia and Care Partners on Challenges, Supports, and Opportunities to Add Geriatric Neuropalliative Care to Dementia Specialty Care
- Harrison KL, Allison TA, et al. "Hospice Staff Perspectives on Caring for People with Dementia: A Multisite, Multistakeholder Study"
- Harrison KL, Garrett SB, et al. "Developing neuropalliative care for sporadic Creutzfeldt-Jakob Disease."
- Harrison KL, Taylor HA, et al. "Action Guide for Addressing Ethical Challenges of Resource Allocation within Community-Based Healthcare Organizations." (dissertation)
- Harrison KL, Taylor HA. "Organizational values in the provision of access to care for the uninsured." (dissertation)
- Harrison KL, Taylor HA. "Healthcare resource allocation decisions affecting uninsured services." (dissertation)
Senior Author
Advance Care Planning and Hospice:
- Hunt LJ, Garrett SB, et al. "'Goals of Care Conversations Don't Fit in a Box': Hospice Staff Experiences and Perceptions of Advance Care Planning Quality Measurement."
- Oh A, Allison TA, et al. "Front-Line Hospice Staff Perceptions of Barriers and Opportunities to Discussing Advance Care Planning With Hospice Patients and Their Families."
- Dressler G, Garrett SB, et al. '"It's Case by Case, and It's a Struggle”: A Qualitative Study of Hospice Practices, Perspectives, and Ethical Dilemmas When Caring for Hospice Enrollees with Full-Code Status or Intensive Treatment Preferences."
Older Adult and Caregiver Experiences and Perspectives:
- Kotwal A, Allison TA et al. "'Relationships, Very Quickly, Turn to Nothing': Loneliness, Social Isolation, and Adaptation to Changing Social Lives Among Persons Living With Dementia and Care Partners."
- Radcliffe KG, Halim M, et al. "Care Setting Transitions for People With Dementia: Qualitative Perspectives of Current and Former Care Partners."
- England AE, Ritchie CS, et al. "Attitudes of Homebound Older Adults and Their Caregivers Toward Research and Participation as Research Advisors."
- Shafir A, Ritchie CS, et al. "'Captive by the Uncertainty'-Experiences with Anticipatory Guidance for People Living with Dementia and Their Caregivers at a Specialty Dementia Clinic."
Collaborations
Care at Home/Homeboundness:
- Sheehan OC, Ritchie CS, et al. "Unanticipated Therapeutic Value of the Patient-Centered Outcomes Research Institute (PCORI) Stakeholder Engagement Project for Homebound Older Adults."
- Mickler AK, Leff B, et al. "Understanding the Daily Experiences and Perceptions of Homebound Older Adults and Their Caregivers: A Qualitative Study."
- Leff B, Sheehan OC, et al. "A Home-Based Care Research Agenda by and for Homebound Older Adults and Caregivers."
Care Ecosystem:
- Bernstein A, Merrilees J, et al. "Using care navigation to address caregiver burden in dementia: A qualitative case study analysis."
- Bernstein A, Harrison KL, et al. "The Role of Care Navigators Working with People with Dementia and Their Caregivers."
- Bock MA, Macchi ZA, et al. "Does a novel community-based outpatient palliative care intervention for Parkinson’s disease and related disorders improve care? Qualitative results from patients and care partners."
- Verma A, Smith AK, et al. "Ethical Challenges in Caring for Unrepresented Adults: A Qualitative Study of Key Stakeholders."
Dementia:
- Bernstein Sideman A, Gilissen J, et al. "Caregiver Experiences Navigating the Diagnostic Journey in a Rapidly Progressing Dementia."
- Allison TA, Gubner JM, et al. "Meaningful Activities and Sources of Meaning for Community-Dwelling People Living with Dementia."
- Bernstein Sideman A, Harrison KL, et al. "Practices, challenges, and opportunities when addressing the palliative care needs of people living with dementia: Specialty memory care provider perspectives."
- Casey JJ, Harrison KL, et al. "An integrative group movement program for people with dementia and care partners together (Paired PLIE): initial process evaluation."
Grief

Overview
Drawing from her personal experiences, Dr. Harrison's work explores the diverse facets of end-of-life care, grief and loss, illuminating the intricate complexities and nuances within this pivotal domain. Her essays underscore the significance of acknowledging grief in academic environments while also delving into the implicit norms prevalent in hospice care. Her research portfolio increasingly reflects this focus. Understanding the multifaceted ways in which grief can affect mental health highlights the importance of providing support and resources to individuals navigating through the complex emotions associated with loss.
Key Publications
- Harrison KL. "Making Space for Grief in Academia, JAMA"
- Harrison KL, Greene M, et al. "We all need help working through grief and hardship."
- Harrison KL. "The Hidden Curriculum of Hospice: Die Fast, Not Slow, Health Affairs"
- Hunt LJ, Harrison KL. "Live Discharge from Hospice Isn’t Graduating - It’s Getting Expelled."
- Gold J. "How to Return to Work with Grief."
Research Impact
Highlighting the significance of addressing grief, Dr. Harrison has identified themes of grief and loss in both qualitative and quantitative data, and reflected findings in her Gerineuropallative Care for Dementia framework:
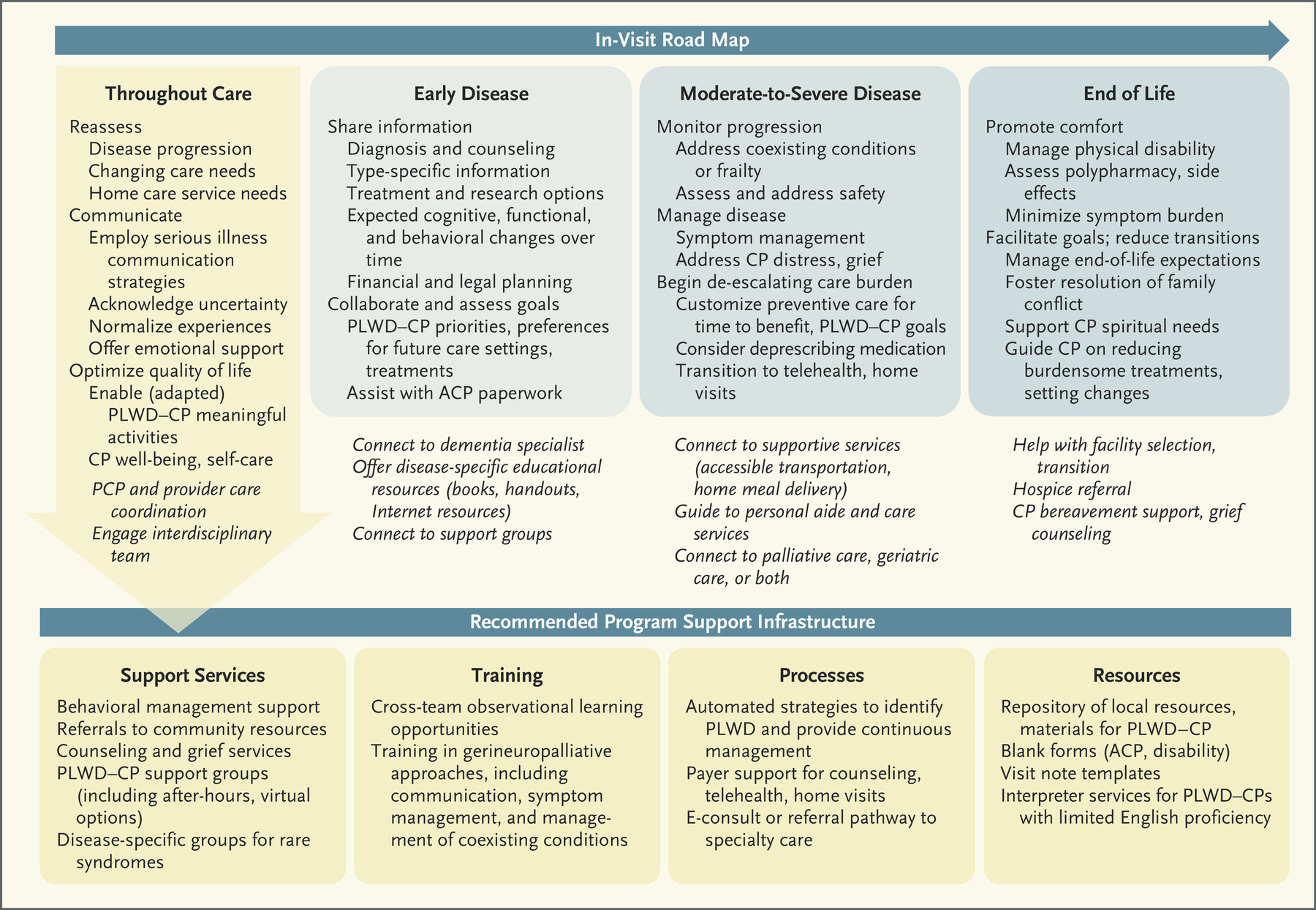
Resources
Through her personal experiences, Dr. Harrison has compiled tools and resources for processing loss and grief. She has been featured on the Health Affairs podcast “Narrative Matters” and as the UNC Grand Rounds Speaker for her talk titled “Adrift at the Dock: Navigating Grief in Serious Illness Care.”
Podcasts Recommendations:




Book Recommendations:




Tips and Support:
Tips for Clinicians
- Embrace a grief-informed approach, paying close attention to signs that indicate the need for additional support.
- Instead of rushing to provide solutions, prioritize therapeutic listening and validation, as these are invaluable in supporting individuals through their grieving process.
- It is beneficial to maintain a list of local resources and seek feedback on their effectiveness.
- Furthermore, develop, test, and implement grief interventions tailored to the specific needs of your patient population.
Supporting Colleagues or Friends
-
Prioritize validation over immediate solutions. Create a supportive environment by actively listening and acknowledging feelings.
-
Extend specific offers of practical assistance tailored to your availability and expertise, such as drafting emails for rescheduling meetings or providing thoughtful gifts like gift certificates, notebooks, neck warmers, or tea.
-
Additionally, offer intangible gifts by respecting communication preferences, sharing updates, sending personalized emails, and consistently reaching out to maintain a strong connection.
Supporting Loss/Grief with Policy
-
Implementation of structured caregiving and compassionate bereavement leave policies
-
Enhanced research efforts focusing on grief studies and effective interventions
-
Integration of specialized grief training programs
-
Expansion of training opportunities, increased funding, and diversified payment methods to enhance the accessibility and quality of grief support services.
Supporting Grievers with Systems
-
Utilize services that specialize in grief to enhance support for employees.
-
Ensure easy access and connection to grief groups for employees in need.
-
Implement grief-informed leadership practices within the organization.
-
Offer paid time off over the first two years to allow employees to grieve and manage death-related administrative tasks, or “dead-min”.
-
Adjust job responsibilities to accommodate grieving employees for 1-2 years after bereavement
-
Provide salary support as a form of assistance during difficult times.
Domains of Research

Dementia
One of the central research domains of the Harrison Network aims to mitigate suffering associated with dementia. An array of qualitative and quantitative studies were carried out to understand needs, support gaps, and identify opportunities to enhance care for individuals with dementia and their care partners.

Hospice Care
As a former leader within a community-based hospice, Dr. Harrison has dedicated her career to enhancing hospice and palliative care through interdisciplinary approaches.

Home-Based Care
Dr. Harrison’s research efforts have focused on developing quality measurements for home-based care, conducting formative qualitative research and stakeholder groups to understand research priorities, and using large datasets to understand the impact of COVID on home-based care.

Health Policy Ethics
Within this research domain, Dr. Harrison's work encompasses health policy ethics and public health ethics at the intersection of marginalized populations impacted by socioeconomic factors or serious illnesses.

Grief
Understanding the multifaceted ways in which grief can affect mental health highlights the importance of providing support and resources to individuals navigating through the complex emotions associated with loss.

Using Qualitative Research in Applied Clinical Research
Qualitative research methodologies enable researchers to explore a diverse range of topics that provide valuable insights into various healthcare and caregiving contexts where quantitative data is unavailable.
Current Research Projects
Here is a collection of ongoing research initiatives aimed at improving care for older adults utilizing a comprehensive approach that blends quantitative, qualitative, and implementation science methodologies.
Improving hospice care for racial and ethnic minoritized older adults with Alzheimer’s Disease and Related Dementias (ADRD)

Project Team
Team: Alexander Smith, MD, MPH, MS, Dan Dohan, PhD, Jennifer James, PhD, MS, MSW, Lauren Hunt, PhD, RN, FNP, Rebecca Sudore, MD
Overview
This 5-year R01-funded study aims to improve hospice and end-of-life care for persons with dementia and their care communities. The project consists of the following three aims:
Aim 1: Understanding Former Caregiver Experiences and Preferences
In this component, we will gather the perspectives of former care partners of persons who died with dementia who identify as Black, African American, Hispanic, Latino/a/x, Asian, Native Hawaiian, Pacific Islander, or multiracial. Through semi-structured interviews and validated survey measures, we will gather experiences of end-of-life care and bias and generate definitions of high-quality end-of-life care, attending to variation within and across identity. This aspect of the research recognizes the diversity of preferences, acknowledging that traditional hospice models may not fully align with the cultural and personal values of these communities.
Aim 2: Examining Organizational Practices
By conducting organizational case studies, we will document hospice practices and policies that influence care for racial and ethnic minoritized persons with dementia. Drawing from surveys, meeting observations, staff interviews, and document reviews, we aim to uncover systemic facilitators and barriers to dementia care within hospice organizations. These findings will be crucial in understanding the structural factors that contribute to disparities in access and quality of care.
Aim 3: Developing Recommendations for Equity
Through collaboration with care partners, policy makers, and experts in hospice and dementia, the project will generate a prioritized set of recommendations for improving equity in hospice care. Building on the insights gathered from aims 1 and 2, this stage will ensure that the proposed recommendations are informed by both the lived experiences of the affected communities and the systemic challenges identified within hospice organizations. The goal is to bridge the gap between current practices and the diverse needs of racial and ethnic minoritized persons with dementia and care partners.
DEploying High ValuE LOngitudinal Population-Based dAta in Dementia Research (DEVELOP AD Research)

This 5 year P01-funded program project supports a series of projects using large secondary data sets (i.e. National Health and Aging Trends Study, Health and Retirement Study, Medicare Care Beneficiary Survey, Medicare Claims) to understand how serious medical illness and social and economic factors impact outcomes in persons with dementia and their caregivers. The project is a joint endeavor between the UCSF Division of Geriatrics and the Department of Geriatrics and Palliative Medicine at Mount Sinai in New York.
UCSF Claude D. Pepper Older Americans Independence (Pepper) Center - Vulnerable Populations Aging Research Core

Alongside Dr. Rebecca Sudore, Dr. Harrison co-directs the UCSF Pepper Center Vulnerable Populations Aging Research Core (VARC) to further develop the UCSF Pepper Center’s initiatives in assisting investigators with designing and executing primary data collection studies involving older adults with medical or social vulnerability.
VARC hosts monthly Office Hours, welcoming all researchers and staff who would like to seek guidance on study design and qualitative/mixed methods analysis.
Health Policy and Public Health Ethics

Research Overview
Within this research domain, Dr. Harrison's work encompasses health policy ethics and public health ethics at the intersection of marginalized populations impacted by socioeconomic factors or serious illnesses. Her studies include examining organizational values in resource allocation for the uninsured and addressing ethical dilemmas in care provision for older adults with serious illnesses.
Team and Funding
This body of work was made possible through funding and support from organizations such as the National Institute of Health (NIH), National Institute on Aging (NIA), National Institute of Nursing Research (NINR), and collaboration with the National Hospice and Palliative Care Organization (NHPCO).
Research Impact
Dr. Harrison's research has made significant contributions to the field of healthcare ethics, particularly in addressing ethical dilemmas related to resource allocation, organizational values, and care provision for vulnerable populations. Her contributions extend to revising ethics guidance for organizations like the National Hospice and Palliative Care Organization (NHPCO) to address concerns in end-of-life care. Dr. Harrison's more recent collaborations delve into ethical dilemmas surrounding care for older adults with serious illnesses.
Key Publications
A sample of our publications within this research domain is categorized into focus areas:
Organizational ethics and allocation of resources for the uninsured
-
Harrison KL, Taylor HA, et al. "Action Guide for Addressing Ethical Challenges of Resource Allocation Within Community-Based Healthcare Organizations."
-
Harrison KL, Taylor HA. "Healthcare resource allocation decisions affecting uninsured services."
-
Harrison KL, Taylor HA. "Organizational values in the provision of access to care for the uninsured."
Care for seriously ill older adults
-
Kirk T, Harrison KL, et al. Guide to Organizational Ethics in Hospice Care.
-
Dressler G, Garrett SB, et al. "'It's Case by Case, and It's a Struggle': A Qualitative Study of Hospice Practices, Perspectives, and Ethical Dilemmas When Caring for Hospice Enrollees with Full-Code Status or Intensive Treatment Preferences."
-
Harrison KL, Dzeng E, et al. "Addressing Palliative Care Clinician Burnout in Organizations: A Workforce Necessity, an Ethical Imperative."
-
Verma A, Smith AK, et al. "Ethical Challenges in Caring for Unrepresented Adults: A Qualitative Study of Key Stakeholders."
-
Portacolone E, Halpern J, et al. "Ethical Issues Raised by the Introduction of Artificial Companions to Older Adults with Cognitive Impairment: A Call for Interdisciplinary Collaborations."
Ethical, legal, social implications of public health or medical interventions
-
Harrison KL, Farrell RM, et al. "'Someone should oversee it': patient perspectives on the ethical issues arising with the regulation of probiotics."
-
Harrison KL, Geller G, et al. "Ethical Discourse about the Modification of Food for Therapeutic Purposes: How Patients with Gastrointestinal Diseases View the Good, the Bad, and the Healthy."
-
Mercer M, Brinich MA, et al. "How patients view probiotics: findings from a multicenter study of patients with inflammatory bowel disease and irritable bowel syndrome."
-
Geller G, Harrison KL, et al. "Ethical challenges in the care of children and families affected by life-limiting neuromuscular diseases."
-
Harrison KL, Errett NA, et al. "An intervention for enhancing public health crisis response willingness among local health department workers: a qualitative programmatic analysis."
-
Barnett DJ, Thompson CB, et al. "EPPM and willingness to respond: the role of risk and efficacy communication in strengthening public health emergency response systems."
